AC-051321-Dark-Angel-DK-7-800
Basic first aid training was once considered sufficient for law enforcement officers. That is no longer the case. When survival is measured in seconds, will you know what to do? Just as we train for worst-case scenarios in shootings, we must also have the medical training for those worst-case medical emergencies, as well.
Emergency medical training should be a basic skill set not just law enforcement, but of every firearms owner. Quite frankly, it should A basic skill set of everyone. The reality is that you are your own first responder. The time to learn what to do kit is not when someone is bleeding out.

The Direct Action Response Training course is hosted at locations around the country. Author attended course at Scottsdale Gun Club, in Scottsdale, Arizona. The Scottsdale Gun Club is a NSSF “Five Star” facility and has been voted “Official Best of Arizona Indoor Shooting Range” five years in a row. Photos by Howard Wack
May is National STOP THE BLEED® Month. To quote the American College of Surgeons, “Often times the person who is right beside a bleeding victim may be the person who’s most likely to save them. That’s why one of the goals of the STOP THE BLEED initiative is to turn civilians into “immediate responders” — a term that describes the first person at the scene of an injury. This person is rarely a trained medical provider.” In today’s world, it’s more important than ever.
This May I attended the Dark Angel Medical Direct Action Response Training™ (D.A.R.T.™), hosted by Scottsdale Gun Club in Scottsdale, Arizona. This was actually the second time that I took the course. I was very impressed with the quality of training the first time around. I wanted to take the course again as a refresher and also to keep my skills current. As with shooting skills, medical skills are perishable skills.
SCOTTSDALE GUN CLUB
Scottsdale Gun Club is a world-class, state of the art community indoor shooting range, training facility and full retail store. It’s recognized by the National Shooting Sports Foundation (NSSF) as a “Five Star Facility.” It has been voted the “Official Best of Arizona Indoor Shooting Range” five years in a row. Home of The Ultimate Shooting Experience™, Scottsdale Gun Club has 32 indoor, air-conditioned 25-yard shooting lanes, including three eight-lane public shooting bays and a tactical bay. It has an expansive retail space/selection including NFA items, full-service gunsmithing, and numerous great training opportunities—both public and private courses.

Direct Action Response Training course was taught by Kerry “Pocket Doc” Davis, founder of Dark Angel Medical. Kerry brought a wealth of real-world experience to the course. He’s an outstanding instructor.

Kerry demonstrating nasal pharyngeal airway placement. Used to maintain airway on unconscious patient. Do NOT use nasal, airway with facial fractures as you may inadvertently place tube in brain tissue.

Kerry discussing individual med kits with two students. A med kit should be lightweight, durable, compact and easy to use. You don’t need to have a mobile trauma room in your kit in order to save a life.
DIRECT ACTION RESPONSE TRAINING
Dark Angel Medical Direct Action Response Training is geared towards those with little to no medical training or background, but also valuable training for those who do. The two-day course is designed to fill the niche between military self-aid/buddy care training and civilian EMS training.
The course provides the student with critical, need-to-know information that can be utilized in a great number of situations. The recent class I attended had a diverse group of students, ranging from a high school student with no prior medical training to a board certified neurologist.
The course consists of a total of 16 hours of classroom work that includes discussion, slide presentations, videos, question and answer sessions, and hands-on practical skills application. A Dark Angel Medical Direct Action Response Handbook training manual, helpful Ten Tac-Med Tips pocket reference card and all necessary training materials for the course are provided to students. The manual and pocket card are the student’s to keep.
Dark Angel Medical Direct Action
Response Training is geared towards those with
little to no medical training or background
Direct Action Response Training will count for certification in Bleeding Control Basics (B-Con) through the American College of Surgeons.
A D.A.R.K.™ (Direct Action Response Kit™) trauma kit may also be purchased at a discount at the time of enrollment. The D.A.R.K. is one of the most well thought out individual med kits available. It has everything you need and nothing you don’t. It’s in keeping with the Dark Angel Medical philosophy of “Simplicity Under Stress.” Students also receive discounts on other Dark Angel Medical products too.
The course I attended was taught by Kerry “Pocket Doc” Davis, founder of Dark Angel Medical. He brings a wealth of practical real-world experience to the course. He’s an outstanding instructor.
KERRY DAVIS
Kerry joined the US Air Force in 1991. He served until 2007, with jobs consisting of Combat Medic/Flight Medic and Officer Training School Instructor. He attended U.S. Army Airborne School at Fort Benning, Georgia while stationed as a flight medic at Pope Field in Fort Bragg, North Carolina. He was deployed in several locations in the Middle East and numerous other locations worldwide with both U.S. and foreign militaries. He subsequently worked as a civilian paramedic and completed his RN. He has worked as a critical care and emergency room RN since 2003.
Kerry is an avid shooter. He has instructed with Magpul Dynamics™ and is currently a part-time instructor with SIG SAUER® Academy, where he teaches tactical medicine programs, as well as firearms classes.
THE D.A.R.T. COURSE
The D.A.R.T. course is quite intensive and covers the following:
Need for training
History of Emergency Care
Ethic and Legality
Physiological and Psychological reactions to environmental stress
Importance of having the proper Combat Mindset
Basic Anatomy and Physiology of life-sustaining systems
HABCDE’s — Hemorrhage, Airway, Breathing, Circulation, “Da Brain” (neurologic), and Expose & Environment.
Breakdown and usage of Individual Med Kit components
Proper stowage and employment of the Individual Medical Kit
Hands-on application of the Individual Medical Kit
Basic and Advanced Airway management — treating and monitoring tension pneumothorax, sucking chest wound and flail chest
Airway adjunct device placement — Nasopharyngeal Airway
Basic First Aid and Advanced wound care
Application of Bandages and Hemostatic Agents
Application of tourniquets
Recognition and Treatment of various injuries (gunshot, laceration, burn, airway, head, orthopedic, environmental)
Recognition and treatment of hypovolemic (hemorrhagic) shock
Moving and positioning victims with various injuries
Response to active shooter situation
Proper use of cover and cover vs. concealment
Casualty recovery in an Active Shooter situation
Mass casualty triage procedure
Emergency Medical Dialect/Lingo (911 protocol, cooperation with First Responders)
Although that’s certainly a lot to cover in a two-day course, the material was presented with professionalism and enthusiasm in an efficient and thorough manner that was conducive to learning. Kerry clearly not only knows his stuff but also how to present it in an engaging way that keeps the students focused.
The training was conducted much as one would build a building. Kerry first laid down the foundation then built the structure on top of the foundation. The slide presentations and videos, many of them quite graphic, and instructor demonstrations reinforced the instruction and drilled the points in, as did the intensive hands-on training which gave the students the opportunity to practice the skills they were taught.
The students were free to ask any questions throughout the course.
The two-day course started promptly at 8:30am and ran until 5:30pm each day, with a one hour break for lunch.
DAY 1
We began our first day covering the need for training, history of emergency care, ethics and legality, and warrior mindset. The right mindset will get you through the toughest situations. We covered combat psychology and the effects of stress and the body alarm response. We learned that the key to success is long term (“train how you bleed”) and the need to stay focused. We also covered the evolution of trauma care in the U.S.
We next moved on to scene safety, situational awareness and the Cooper Color Code System. The common factors that can impact good situational awareness, such as protective gear, low light conditions and environmental factors were also discussed, as well as the importance of personal protective equipment (PPE). Personal safety trumps everything else. Options to preserve our safety while still providing patient care were discussed. It does no one any good for use to become another patient. Sometimes hard decisions have to be made.
We then moved on to basic anatomy and physiology. The H A B C D E’s [Hemorrhage, Airway, Breathing, Circulation, “Da Brain” (Neuro), and Expose and Environment) were the areas of focus. We learned how to assess a patient and identify and treat the most life threatening injuries.
HEMORRHAGE
Early on in the course, Kerry began to explain the importance of tourniquets and the various types. Roughly 80% of combat deaths and 50% of civilian trauma deaths are attributable to hemorrhage. It’s the most preventable cause of death in compressible injuries. The proper use of tourniquets save lives. We also learned wound packing, and the types and use of hemostatic agents and pressure dressings.
Roughly 80% of combat deaths and 50% of civilian
trauma deaths are attributable to hemorrhage. It’s the most
preventable cause of death in compressible injuries.
Every student was provided with a blue Combat Application Tourniquet® (CAT®) trainer on loan at the beginning of the class. At random intervals throughout the course Kerry would call out “tourniquet” and a specific limb for us to apply it. It became a race to who of us could be the first to properly apply the tourniquet to our own limb. We also took the tourniquet home with us overnight to practice further with it. Needless to say, all of us became quite proficient.
AIRWAY & BREATHING
After we dealt with treating massive blood loss, we moved onto the respiratory system. We learned to identify whether or not our patient had a patent airway (open and maintainable airway). We studied the anatomy of the respiratory system and common airway and breathing injuries that could arise as a result of trauma and how to treat them. As the brain has a constant need for oxygen, it’s vital that we get the patient breathing and oxygenated blood circulating as quickly as possible.
The types and use of artificial airways, artificial respiration, barrier devices and occlusive dressings (and field expedients) were covered. C-spine precautions and C-spine control, the recovery position, and special considerations were also covered.

Kerry demonstrating wound packing to a very attentive City of Glendale (AZ) K9 Ranger and his handler Chris Kurtzhals. Goal is to pack the “wound bowl” down to the bone, occluding the artery, and create focused pressure on the hemorrhage. Ranger obviously enjoyed the course.

Student practicing wound packing with hemostatic gauze under watchful eyes of Kerry. We practiced applying different types of tourniquets, packing wounds, applying direct pressure and pressure bandages.
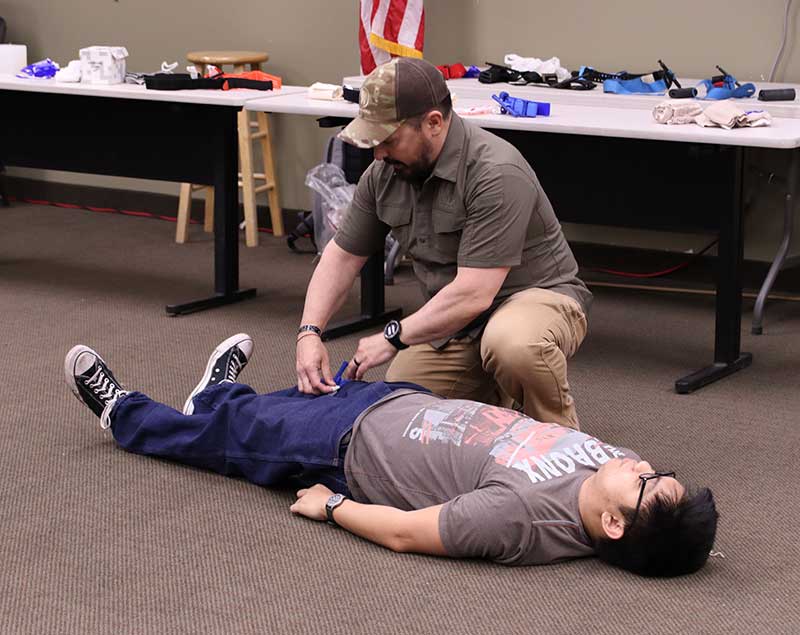
Kerry applying CAT trainer to student. Tourniquets are used for rapid control of life-threatening bleeding. May need more than one. Hemorrhage is the most preventable cause of trauma deaths.
CIRCULATION
After any massive bleeding has been stopped and our patient’s breathing has been assessed, we need to make certain the blood is circulating throughout the body. We studied the anatomy of the circulatory system and learned how to the assess and interpret pulses from various points on the body, skin temperature, color and capillary refill. The importance of thoroughly reassessing the patient periodically or if the condition deteriorates was also stressed.
The body is a hydraulic machine. The blood is the body’s hydraulic fluid. As emergency caregivers, we must keep as much of the patient’s blood inside the body as possible and to ensure that it’s circulating properly.
“DA BRAIN,” EXPOSE & ENVIRONMENT
We then covered anatomy and physiology of the neurological system. We learned how to assess the Level of Consciousness (LOC). The importance of constantly reassessing metal status was stressed. An altered level of consciousness can be an early indicator of “things going bad.” Any deficit in blood, sugar and oxygen will present in the form of an altered LOC.
After that we covered the last step in the assessment process, which is to expose the patient to assess for any further injuries. You don’t want your patient to die due to a lack of attention to detail. After exposure and assessment it is important to think of environment. Cover the patient up and keep them warm.
SPECIFIC INJURIES
We then moved on to specific injuries and how to diagnose and treat them. There is no hard and fast rule in trauma+. The situation and injury will dictate the treatment. Injuries were broken down into three injury categories—minor injuries, emergent injuries, and environmental injuries.
MINOR INJURIES
Minor injuries covered included:
Lacerations
Avulsions
Contusions
Abrasions
Fractures
EMERGENT INJURIES
Emergent injuries are severe, sudden traumatic injuries. They can be immediately life threatening. They may be combination injuries. Emergent injuries covered included:
Gunshot Wounds
Stabbing/Impaled Objects
Amputations
Blast Injuries
Chest Trauma, including flail chest, sucking chest wound & tension pneumothorax
Facial Injuries compromising airway
Eviscerations
Hypovolemic Shock, Anaphylactic Shock
DAY 2
The second day of the course started with a discussion of environmental injuries. Environmental injuries are often overlooked. They are easy to prevent, but can have serious, immediately life threatening consequences. They include toxins, heat and cold injuries. Environmental Injuries that were covered included:
Poisonous Plants
Snakebites
Creepy Crawlies
Carbon Monoxide
Thermal Injuries, including Heat Exhaustion, Heat Stroke, Burns, Frostnip, Frostbite, Hypothermia
The amount of detail and time spent in on type of injury each varied, with the greatest emphasis on traumatic injuries and those injuries that could be immediately life threatening. Pediatric and K9 injuries were also discussed. Rather than memorizing one action for each injury as taught in many first aid courses, we learned that common treatment modalities can address multiple injuries, a trauma treatment force multiplier, if you will. A few different techniques can be utilized in multiple combinations. Once again, this is where our understanding of anatomy and physiology came into play.
INDIVIDUAL MEDICAL KIT
Kerry then went over the Individual Medical Kit (IMK). Many of the students had purchased the D.A.R.K. from Dark Angel Medical. Kerry went over each of the components in the kit and why they were included. Many of the components have “other capabilities” than their primary purpose. We were given examples of how they may be used. For those that didn’t purchase the kit, some time was also spent on putting together one’s own kit. Each of the components was covered in depth. For example, you should always use nitrile gloves since many people have a latex allergy and can go into anaphylactic shock as a result of contact with latex.

Student role playing. Every student got the chance to play both patient and emergency caregiver. Kerry assessed and debriefed students on patient assessment and treatment.

Kerry demonstrating use of compression bandage for head wound on head of student. Pressure bandage is used to direct and maintain pressure on wound.
VICTIM MOVEMENT & ADDITIONAL CONSIDERATIONS
Victim positioning and movement, cover vs. concealment and additional considerations such as low light environments, NBC/HAZMAT operations, 911 communication, guidelines for triage, and critical incident stress management were covered next.
Incidents may have more than one victim. Triage prioritizes treatment. A modified HABCDE assessment is used to sort the victims. Triage uses a nationally standardized color code system: Green ,Minimal (walking wounded); Red, Immediate; Yellow, Delayed; and Black or Blue, Expectant (nothing can be done to save). In a tactical low light environment, colored light sticks are often used to tag victims. The most important thing to remember is “do the most good for those you can help.”
Kerry also provided recommendations for further reading and additional training, as well additional resources.
HANDS-ON TRAINING
Hands-on skill stations were then set up in the classroom. We practiced inserting the Nasopharyngeal Airway (NPA) after measuring its correct length (on an airway management trainer, not on students). We practiced applying different types of tourniquets, packing wounds (on a Phokus Wound Cube™), applying direct pressure and pressure bandages. We also practiced splinting and tying a sling and swathe. Kerry was always around to guide us and answer any questions. After we had rotated through all the hands-on skill stations, we all felt quite confident in our abilities.
Finally, each of us was paired up with another student, where we practiced our assessment and treatment skills on each other. We each had the opportunity to play emergency caregiver and victim. The victim or Kerry chose the injury. Kerry evaluated and critiqued our performance. It was an excellent learning process.
At the end of the course, each student who successfully completed the training was awarded a Dark Angel Medical Direct Action Response Training Certificate of Completion, Bleeding Control (B-Con) Certification and a very cool Dark Angel Medical challenge coin.
CONCLUSION
Dark Angel Medical Direct Action Response Training is outstanding, well thought out training. Everyone who attended had the highest praise for the course. I highly recommend it. The training you will receive is invaluable. It may save your life or that of a loved one.
The course is hosted throughout the year at various locations around the country. The cost is $420 ($475 in Alaska) and worth every single penny. To register for a course or for information on hosting a course, contact Dark Angel Medical or visit their website.
DARK ANGEL MEDICAL, LLC
(720) 836-7150
www.darkangelmedical.com
SCOTTSDALE GUN CLUB
(480) 222-4351
www.scottsdalegunclub.com